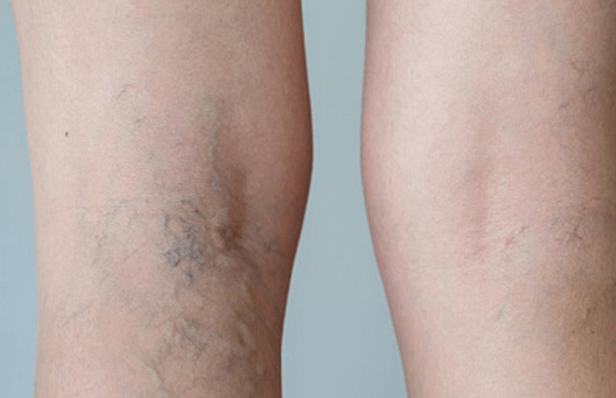
 As people age, they begin to notice an increase in tiny, damaged, twisted and swollen capillaries at the surface of their skin. These red and sometimes blue or purple blood vessels are commonly called spider nevus or spider veins because of their web-like spread across the skin.
As people age, they begin to notice an increase in tiny, damaged, twisted and swollen capillaries at the surface of their skin. These red and sometimes blue or purple blood vessels are commonly called spider nevus or spider veins because of their web-like spread across the skin.
Although they often appear on the face and legs, they can occur naturally anywhere on the skin from normal physical and circulation changes related to the expansion and contraction of the vessels. In many cases, spider veins are nothing more than a cosmetic problem, but they can also be a warning sign of a serious underlying medical condition. Seniors are at higher risk of spider veins appearing for a variety of reasons. As a result, it's important that they review this guide and speak with a doctor if they notice an increasing number of spider veins on their body..
Main Causes of Spider Veins
Beyond the natural wear and tear that weakens blood vessels over time, a wide range of additional factors can lead to the formation and enhanced appearance of spider veins.
Family History
Many people are genetically predisposed to having spider veins or conditions that can cause or exacerbate enlarged capillaries. They might have a family history, for example, of structurally weak or defective blood vessels, high blood pressure or poor overall circulation. If they have a family history of large varicose veins or leg blood clots, the chance of spider veins increases because of blood flow problems leading from those veins.
Pressure Variations
Any time pressure changes in or around the capillaries, their inner and outer walls expand and contract. High blood pressure, weight gain and swelling from all-day activity can put too much pressure on the blood vessels. Over time, that pressure leads to wall weakness. This can also happen when a person decreases and then rapidly increases blood flow by sitting in one position for too long, such as when sitting in an office chair with their legs bent at 90 degrees or in a relaxation pose with one leg up under the other. That said, time isn't the only factor. Simply blowing your nose or a sneeze will cause spider vein formation if the vessels are thin or weak.
Physical Defects
Beyond genetic vessel weakness, other types of physical defects can weaken vessels or cause pressure variations. For example, twisted or "tortuous" blood vessels have dilated and constricted sections. Twists and even bends in a blood vessel can cause blood to stop flowing correctly at different points in the circulatory system. Any large blood vessel constriction, also known as vasoconstriction, can result in sudden slow or fast blood flow, as can low and high blood pressure situations depending on other factors like movement and blood pressure. This is similar to how the flow of a beverage decreases and increases depending on how someone handles a drinking straw. Additionally, a person might have scar tissue from an old injury or surgery that is affecting nearby blood vessels.
Physical Damage
Any type of damage to the skin and blood vessels can result in spider veins because of sudden or slow damage to the vessel walls, blood flow, and/or pressure changes. For example, many seniors accidentally bump their legs. After the swelling and bruising disappear, they find spider veins. Additional physical damage can occur from windburn, scrapes, attempts to "pop" acne, rubbing the face or legs repeatedly over the course of a day, falls and other injuries.
Thin Skin
Seniors often describe having "thin skin" that bruises "easily." As people age, two main proteins that help skin to stay firm and strong, elastin and collagen, break down and the skin does actually become thin and weaker. Not only are blood vessels more easily damaged, but seniors can then also see blood vessels that are close to the surface more clearly. Of course, some people are merely born with thinner skin. Plus, sunburns that cause the skin to peel can create the same effect at any age.
Hormonal Changes
After puberty, men and women's bodies continue experiencing hormonal changes for the rest of their lives. Inflammation in the body and weight gain can increase while blood vessels want to enlarge, expand and contract more than usual during periods of severe hormonal changes, such as pregnancy and menopause in women. Taking a hormonal supplement, whether prescribed or over-the-counter, can have a similar impact.
Increased Inflammation
Inflammation causes swelling in the body that can then cause vessel-related pressure damage. The inflammation can also push veins closer to the surface of the skin. Prolonged sun exposure and hot weather causes inflammation and swelling as well. Plus, some anti-inflammatory medications actually increase blood pressure by affecting water retention and the kidneys.
Other Causes
Several organ diseases affect the capillaries. For example, the flushing and inflammation seen when someone has rosacea results in many people with this skin disease having spider veins on their faces. When fat builds up in the liver from fatty liver disease, blood flows sluggishly or clots, which impacts blood pressure. Spider veins in people with fatty liver disease appear frequently on the face, shoulders and back. They also frequently appear on people who are receiving cancer-related chemotherapy and radiation treatments that have side effects which cause physical damage, inflammation, circulation issues, etc.
When Is It Time to Speak to a Doctor?
Certain types of at-home preventative actions can reduce the formation and appearance of spider veins for people with no serious underlying health conditions. For example, since caffeine and alcohol both cause the dilation of blood vessels, seniors should consider reducing their intake of these substances, in particular alcohol as it’s well known to damage the liver. A good sunscreen, broad-rimmed hat, and limiting sun exposure to intervals of 10 to 15 minutes can reduce sun-related inflammation and skin damage. A moisturizer and cream enriched with vitamin A to help boost collagen, for example, can make the skin stronger, healthier and more durable. Seniors should also move around more often and prop up their legs when sitting or resting on a recliner or couch.
Depending on their location, size, and number, spider veins can be rather unsightly. Like varicose veins, which are merely larger blood vessels experiencing similar problems, they can also increase discomfort by inflaming sections of skin, making them swollen to the touch.
It's definitely time to see a doctor if their appearance or related sensations are causing you discomfort -- even if it's only unhappiness. Many seniors suffer from feelings of sadness and depression. A better outward appearance and less irritation can boost mood. Seniors should also speak with a doctor if the appearance of new spider veins seems to increase in a short period of time, or should they feel unusually tired, weak, physically heavier or bloated, or simply feel “off” in general. In addition, a senior should schedule an emergency appointment if they experience yellowing of the eyes or skin, which indicates liver failure. A physician will then perform a series of diagnostic tests based on a patient's specific symptoms and offer one or more treatment solutions. For cosmetic and non-life-threatening situations, a doctor might recommend a laser treatment that shrinks the vessels, or a drug that improves the state of the vessels or deals with inflammation. For more severe situations, any treatment approach will depend on the underlying condition.


Comments